AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Pathological complete response8/12/2023 
2 Patients with a recurrence score ≥ 25 received docetaxel plus cyclophosphamide, while those with recurrence score ≤ 10 received exemestane patients with recurrence score ranging from 11 to 24 were randomly assigned between these arms. Zelnak compared chemotherapy to endocrine neoadjuvant therapy in a pilot study of 46 patients stratified by 21-gene recurrence score. “We are struggling with how to downstage these cancers,” Dr. O’Regan commented.Įstrogen receptor–positive cancers are the least responsive to neoadjuvant chemotherapy and need alternative treatments in the preoperative setting. “The point is, if we really believe that pCR is the gold standard for outcome, we have a lot of patients who, unfortunately, don’t achieve it,” Dr. HER2-positive cancers have a better chance, especially the hormone receptor–negative subset, and approximately one-third of patients with triple-negative breast cancer achieve pCR. 1 In general, hormone receptor–positive cancers (luminal A and B) have the least chance of a pCR after neoadjuvant chemotherapy, especially if they are low-grade. The recent meta-analysis by Cortazar et al illustrates the huge variability in pathologic complete response by breast cancer subtype. Since that time, the issue of pathologic complete response-who achieves it, what it means-has become infinitely more nuanced. Zelnak noted that the early preoperative trials-especially National Surgical Adjuvant Breast and Bowel Project (NSABP) B-18 and B-27-showed that patients achieving a pathologic complete response had better long-term outcomes, but these early data were not broken down by HER2 or hormone receptor status, and were conducted before intrinsic subtyping entered the picture. There are patients who achieve a pCR who still have recurrences, and many others who don’t achieve a pCR and still do wellĭr. We need to be careful about how we discuss this with them. 
Zelnak, MD, Assistant Professor of Hematology and Medical Oncology at Emory, added, “As we use more and more neoadjuvant therapy, our patients are really attuned to how the treatment is working. O’Regan, MD, Professor of Hematology and Medical Oncology at Emory University and Chief of Hematology and Medical Oncology at the Georgia Cancer Center for Excellence at Grady Memorial Hospital, Atlanta.Īmelia B. “It’s complicated, but pathologic complete response is not predictive of outcome for the majority of breast cancers,” said Ruth M. Patients are increasingly interested in this outcome, but it means different things to different patients, according to two breast cancer specialists from Emory University, who discussed the meaning of pCR at the Debates and Didactics in Hematology and Oncology meeting in Sea Island, Georgia. In the neoadjuvant treatment of breast cancer, the importance of achieving a pathologic complete response (pCR) varies substantially by breast cancer subtype. There are patients who achieve a pCR who still have recurrences, and many others who don’t achieve a pCR and still do well long-term. 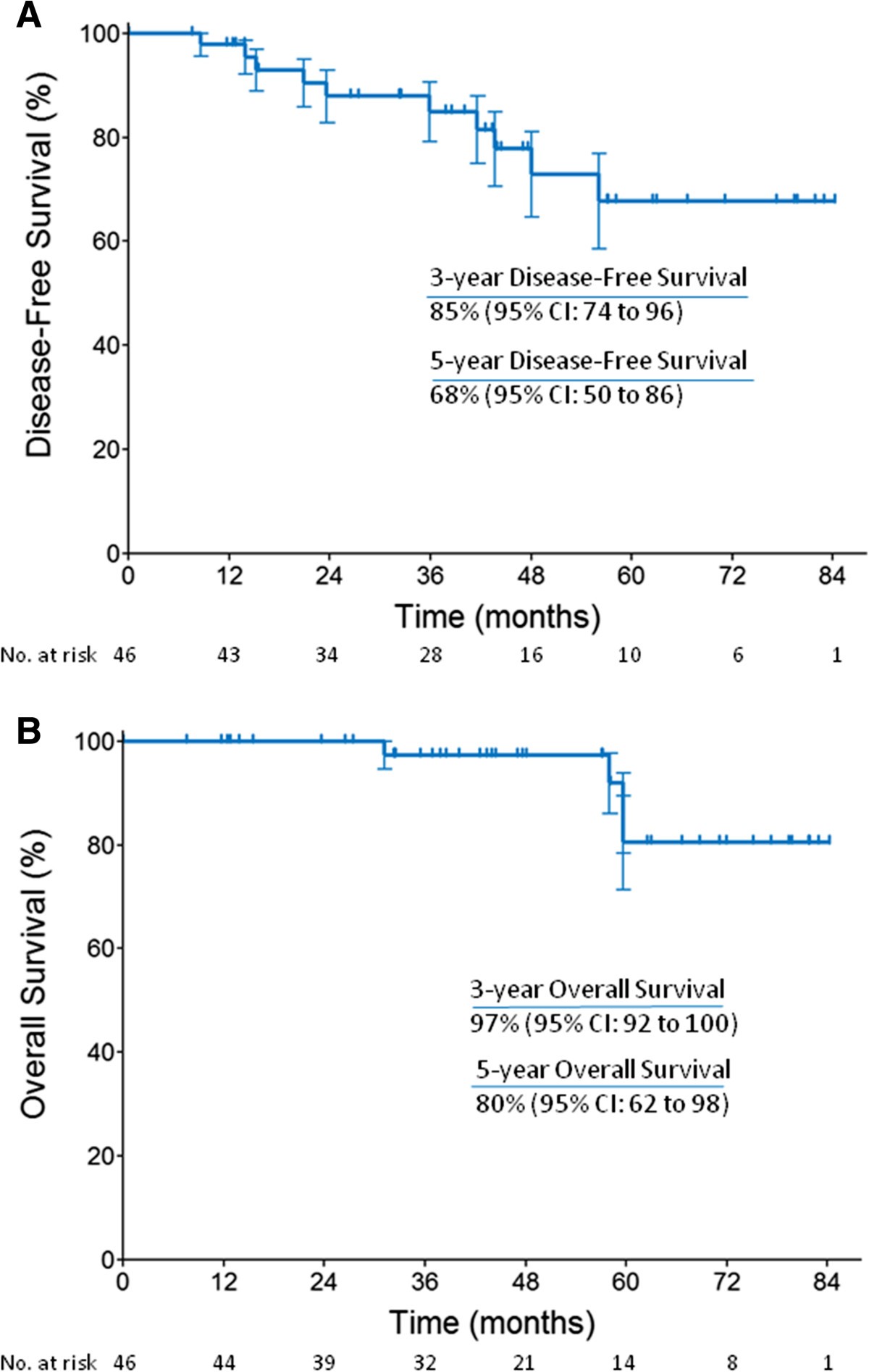
It’s complicated, but pathologic complete response is not predictive of outcome for the majority of breast cancers. Pathologic Complete Response in Breast Cancer
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
